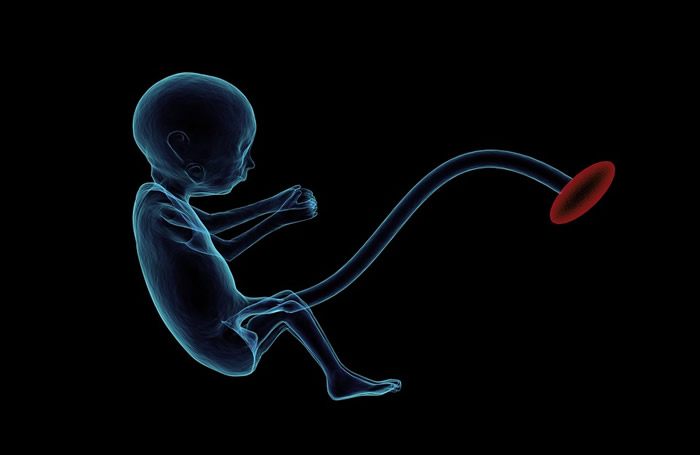
Mothers with diabetes will find that their blood flows preferentially to the placenta instead of the brain in fetuses.
The research behind this was presented recently at EuroEcho-Imaging 2016.
Lead Author Dr Aparna Kulkarni, a Paediatric Cardiologist from the Bronx-Lebanon Hospital Center, New York, USA, said: “We know that maternal diabetes mellitus affects the fetal organs. Babies born to mothers with diabetes are sometimes bigger, especially if the diabetes is uncontrolled, and the placenta is larger. There is data to suggest that some other organs such as the pancreas and the kidneys in the fetus might be affected.”
Dr Kulkarni’s previous research identified subclinical changes in the heart muscle of fetuses of mothers with diabetes. In the current study she investigated whether these foetuses had changes in blood circulation.
This study included 14 fetuses of mothers with type 1 or 2 diabetes and a control group of 16 fetuses of mothers without diabetes. Nine of the diabetic mothers used insulin, three took oral medications, and two used diet alone to control their glucose levels.
The researchers used fetal Doppler echocardiography to measure blood flow to the brain, the left and right outflow tracts of the heart, the aorta, and the placenta. The data was plugged into a computerized model that mimics the fetal circulation. This model was developed by Dr Patricia Garcia-Canadilla in the Physense research laboratory of Dr Bart Bijnens at the University of Pompeu Fabra, Barcelona, Spain.
This research found that, compared to fetuses in the control group, in fetuses of diabetic mothers more blood flowed to the placenta and was diverted away from the brain. Specifically, fetuses of diabetic mothers had lower placental resistance and compliance, lower blood flow to the arteries in the brain (measured from the cerebral artery radius), a reduced proportion of blood flow to the brain than the placenta and a lower cardiac output.
Dr Kulkarni said: “The computational model equivalent of the fetal circulation is an electrical circuit where there are resistances and compliances. It is easier for blood to flow to the placenta, and harder for blood to flow to the brain.”
Dr Kulkarni said the placenta in fetuses of diabetic mothers have changes in their blood vessels and are known to be large; therefore likely receive more blood supply. But she added that the lower proportion of blood supplying the brain is an interesting finding and could have bigger implications.
“The placenta gets taken away after a baby is born so it’s no longer a part of the circulation,” she said. “But it’s possible that the reduced circulation to the brain in utero could affect the baby through life. We don’t know enough about why this redistribution of blood flow occurs or the implications it might have. More research is needed to find out if this has any long-term impact on the health of the baby and whether anything can be done to prevent it.”
Dr Kulkarni concluded: “At the present time, I don’t think any changes should be made in management of pregnant women with diabetes mellitus based on these findings. Standard obstetric recommendations for strict glucose control and healthy lifestyle should be continued.”
More information: EurekAlert!